CALL TODAY 646-846-1136 | EMAIL
Surgical Experts Dedicated to Improving Lives
At Lenox Hill Minimally Invasive Surgery PLLC, Dr. Valery Dronsky and his staff of medical professionals provide compassionate care with the highest ethical & professional standards. In our state of the art facility, we offer surgical services using only the most cutting edge and current procedures and treatments. We specialize in general surgery, including extensive experience in performing hernia repair surgery. Our expertise is in minimally invasive surgery and robotic surgery. Minimally invasive and robotic surgery often allow patients to experience easier recovery than traditional open surgery. They also allow for more precise and less traumatic surgery. When robotic and minimally invasive surgery is not an option, we are also skilled and experienced in traditional open surgical procedures.
Dr. Dronsky is an experienced and highly skilled surgeon having undergone extensive training in school, residency and fellowships. He practices medicine with ethical behavior, compassion and superb bedside manner. In the operating room he exhibits precision mechanical abilities, analytical thinking and the ability to visualize tissue in three dimensions. These innate and learned skills allow Dr. Dronsky to be one of the most dexterous and skilled professionals in New York City and the Country.
Call us: 646-846-1136
PATIENT TESTIMONIALS
Recent Awards
We are honored and deeply appreciative to have consistently received prestigious awards and recognition year after year, establishing us as one of New York’s foremost hospitals for a wide range of general surgeries, safety measures, specialized procedures, and overall excellence in healthcare. At Lenox Hill Minimally Invasive Surgery, our unwavering commitment lies in delivering exceptional care and unwavering support to our patients, guaranteeing their safety and successful recovery throughout their entire surgical experience.
Hospital Quality Awards
 America’s 50 Best Hospitals Award™ (2023, 2022)
America’s 50 Best Hospitals Award™ (2023, 2022)
Top 1% in the nation for providing the highest clinical quality year over year.

America’s 100 Best Hospitals Award™ (2021)
Top 2% in the nation for consistently delivering clinical quality year over year.

America’s 250 Best Hospitals Award™ (2023, 2022, 2021)
Top 5% in the nation for consistently delivering clinical quality.

Patient Safety Excellence Award™ (2023, 2022)
Top in the nation for providing excellence in patient safety by preventing infections, medical errors, and other preventable complications.
Specialty Clinical Quality Awards

America’s 100 Best Hospitals for Cardiac Care Award™ (2023, 2022, 2021, 2020, 2019)
Superior clinical outcomes in heart bypass surgery, coronary interventional procedures, heart attack treatment, heart failure treatment, and heart valve surgery.

America’s 100 Best Hospitals for Coronary Intervention Award™ (2023, 2022, 2021, 2020, 2019)
Superior clinical outcomes in coronary intervention procedures (angioplasty with stent).

America’s 100 Best Hospitals for Prostate Surgery Award™ (2023, 2022, 2021)
Superior clinical outcomes in prostate removal surgery and transurethral resection of the prostate.
Click to see all of our Healthgrades best doctors awards


Visit our main website at www.LenoxHillMinimallyInvasiveSurgery.com
Blog Posts are Below:
Monthly Archives: December 2025
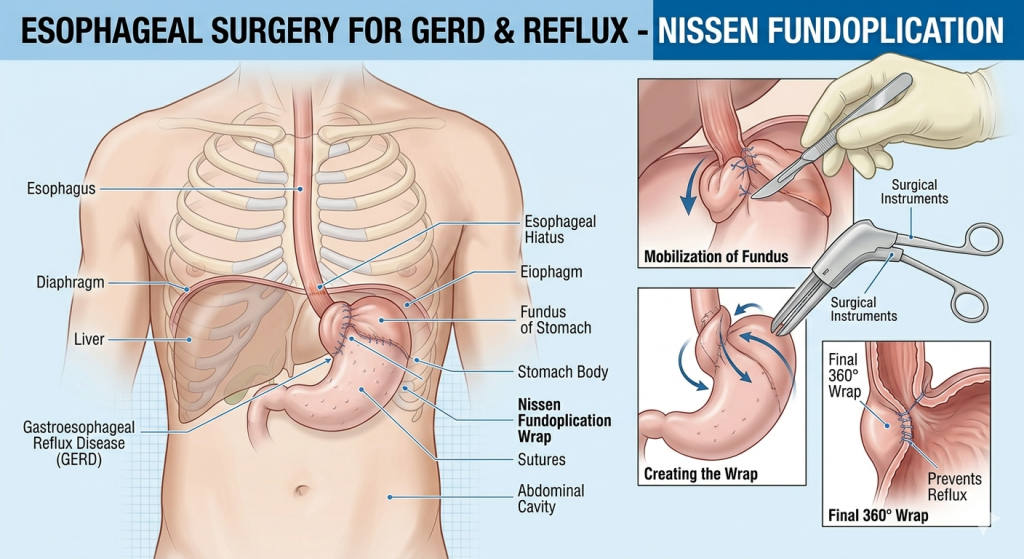
Esophageal Surgery for GERD and Reflux: Is a Fundoplication Right for You?
Esophageal surgery for GERD and reflux may be recommended when chronic acid reflux no longer responds to medications or lifestyle changes. Gastroesophageal reflux disease (GERD) affects millions of people and occurs when stomach acid frequently flows back into the esophagus, causing irritation and inflammation. While many patients manage GERD with medications such as proton pump inhibitors, others experience persistent symptoms that require surgical treatment. One of the most effective surgical procedures for GERD is fundoplication, which helps restore the normal barrier between the stomach and esophagus.
Understanding GERD and Chronic Acid Reflux
GERD develops when the lower esophageal sphincter (LES)—the muscular valve between the esophagus and stomach—becomes weak or relaxes inappropriately. This allows stomach acid to move upward into the esophagus.
Common symptoms of GERD include:
- Persistent heartburn or burning sensation in the chest
- Regurgitation of food or sour liquid
- Difficulty swallowing (dysphagia)
- Chronic cough or throat irritation
- Hoarseness or voice changes
- Chest discomfort after meals
Left untreated, chronic reflux can damage the lining of the esophagus and lead to complications such as esophagitis, strictures, or Barrett’s esophagus.
When Is Surgery Recommended for GERD?
Most GERD patients initially receive treatment through lifestyle changes and medications. However, surgery may be recommended in certain situations.
- Persistent symptoms despite long-term medication use
- Dependence on acid-reducing medications for symptom control
- Severe reflux causing inflammation or ulcers in the esophagus
- Complications such as Barrett’s esophagus
- Presence of a large hiatal hernia
- Patients who prefer a long-term surgical solution instead of lifelong medication
Surgical treatment can provide durable symptom relief and improve quality of life.
What Is Fundoplication Surgery?
Fundoplication is the most common surgical procedure used to treat GERD. During this procedure, the upper portion of the stomach (the fundus) is wrapped around the lower end of the esophagus.
This wrap strengthens the lower esophageal sphincter and prevents stomach acid from flowing back into the esophagus.
Types of fundoplication procedures include:
- Nissen fundoplication: A complete 360-degree wrap around the esophagus
- Toupet fundoplication: A partial wrap used in select cases
- Dor fundoplication: Another partial wrap sometimes used with other esophageal procedures
Your surgeon will determine which technique is most appropriate based on your condition and anatomy.
Minimally Invasive Fundoplication
Today, most fundoplication procedures are performed using laparoscopic or robotic-assisted techniques.
During minimally invasive surgery:
- Several small incisions are made in the abdomen
- A camera provides high-definition visualization of the surgical area
- Specialized instruments are used to create the stomach wrap
Benefits of minimally invasive surgery include:
- Less postoperative pain
- Smaller scars
- Shorter hospital stays
- Faster return to daily activities
- Reduced risk of infection
These advantages make minimally invasive fundoplication a popular option for many patients in NYC.
How to Know If You Are a Candidate
Before recommending surgery, doctors typically perform several diagnostic tests to confirm GERD and evaluate esophageal function.
- Upper endoscopy: Allows visualization of inflammation or damage to the esophagus
- Esophageal pH monitoring: Measures acid exposure in the esophagus
- Esophageal manometry: Evaluates muscle function and swallowing
- Imaging studies: May identify hiatal hernias or structural abnormalities
These tests help ensure surgery will effectively relieve symptoms.
Recovery After Fundoplication Surgery
Recovery after minimally invasive fundoplication is usually relatively quick.
- Most patients stay in the hospital for one day or less
- A temporary soft or liquid diet is recommended
- Normal activities can often resume within 1–2 weeks
- Heavy lifting should be avoided for several weeks
Many patients experience significant improvement or complete resolution of reflux symptoms after surgery.
Potential Risks and Side Effects
Fundoplication surgery is generally very safe, but as with any operation, certain risks exist.
- Difficulty swallowing during early recovery
- Bloating or gas
- Infection or bleeding
- Rarely, recurrence of reflux symptoms
Most side effects improve as healing progresses.
Long-Term Results of GERD Surgery
For many patients, fundoplication provides long-term relief from reflux symptoms and eliminates the need for daily acid-reducing medications. Studies show that the majority of patients experience significant improvement in quality of life following surgery.
However, ongoing follow-up with your surgeon and gastroenterologist remains important for monitoring long-term digestive health.
Conclusion: When Surgery Can Provide Lasting Relief
Esophageal surgery for GERD and reflux offers an effective solution for patients whose symptoms cannot be controlled with medication alone. Fundoplication strengthens the natural barrier between the stomach and esophagus, helping prevent acid reflux and protect the esophagus from long-term damage.
With modern minimally invasive techniques, patients can achieve excellent results with shorter recovery times and minimal disruption to daily life.
Contact Information
LENOX HILL MINIMALLY INVASIVE SURGERY LLP
155 East 76th Street
New York, NY 10021
Tel: 646-846-1136
Email: lenoxhillsurgeons@gmail.com
Visit us online: https://www.lenoxhillminimallyinvasivesurgery.com
Small Bowel Obstruction Surgery: When Emergency Intervention Is Required
A small bowel obstruction (SBO) is a serious medical condition that occurs when the normal passage of contents through the small intestine becomes blocked. This blockage can lead to severe abdominal pain, vomiting, dehydration, and potentially life-threatening complications if not treated promptly. While some cases can be managed with non-surgical treatments, others require urgent or emergency surgery to restore normal bowel function.
For patients in NYC, understanding the causes, warning signs, and treatment options for small bowel obstruction can help ensure timely medical care and improved outcomes.
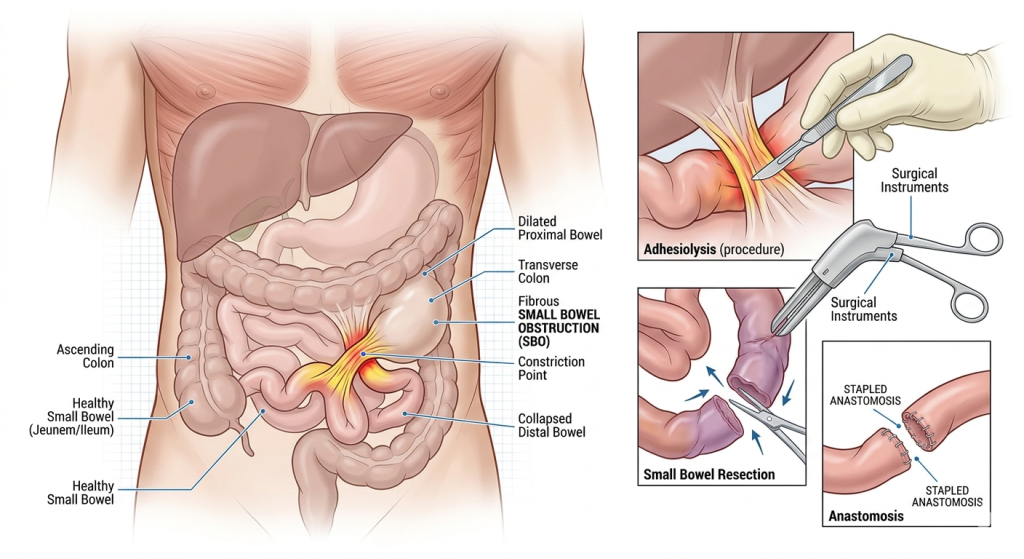
What Is a Small Bowel Obstruction?
The small intestine is responsible for absorbing nutrients and transporting digested food through the digestive tract. When a blockage occurs, food, fluids, and gas cannot move normally through the intestines.
This obstruction may be partial or complete, and it can occur suddenly or develop gradually over time.
Common Causes of Small Bowel Obstruction
Several conditions can lead to a blockage in the small intestine.
- Abdominal adhesions: Bands of scar tissue that form after previous surgery are the most common cause.
- Hernias: Portions of the intestine may become trapped in a weakened area of the abdominal wall.
- Tumors: Both benign and malignant growths can obstruct the bowel.
- Inflammatory bowel disease: Conditions like Crohn’s disease can narrow sections of the intestine.
- Twisting of the intestine (volvulus): This can cut off blood supply and create a surgical emergency.
- Intussusception: One segment of intestine slides into another, causing blockage.
Identifying the underlying cause is critical in determining the most appropriate treatment.
Symptoms of Small Bowel Obstruction
Symptoms often develop quickly and may worsen over time. Common warning signs include:
- Severe abdominal pain or cramping
- Nausea and persistent vomiting
- Abdominal bloating or swelling
- Inability to pass gas or have a bowel movement
- Loss of appetite
- Dehydration and fatigue
If the obstruction cuts off blood flow to the intestine, symptoms may become more severe and require immediate surgery.
How Small Bowel Obstruction Is Diagnosed
Doctors use a combination of physical examination and imaging tests to diagnose SBO.
- CT scans: The most common imaging test used to identify the location and cause of obstruction.
- Abdominal X-rays: May show air-fluid levels indicating a blockage.
- Blood tests: Used to evaluate infection, dehydration, and electrolyte imbalances.
Early diagnosis allows doctors to determine whether surgery is necessary.
Non-Surgical Treatment Options
In some cases, especially partial obstructions, doctors may attempt non-surgical management first.
- Hospital observation and monitoring
- Intravenous fluids to treat dehydration
- Nasogastric tube placement to decompress the stomach
- Bowel rest (no food or drink temporarily)
If the obstruction resolves, surgery may be avoided. However, if symptoms worsen or fail to improve, surgical intervention becomes necessary.
When Is Emergency Surgery Required?
Emergency surgery is required when:
- The obstruction is complete
- Blood supply to the intestine is compromised
- There is bowel perforation or infection
- Non-surgical treatment fails
- The patient develops severe or worsening symptoms
Prompt surgery can prevent serious complications such as tissue death (necrosis) or life-threatening infection.
Surgical Treatment for Small Bowel Obstruction
The goal of surgery is to remove the blockage and restore normal intestinal function.
Depending on the cause, surgery may involve:
- Removing adhesions causing the obstruction
- Repairing a hernia trapping the intestine
- Removing a tumor blocking the bowel
- Untwisting the intestine in cases of volvulus
- Resecting damaged portions of bowel if blood supply has been compromised
Minimally Invasive vs. Open Surgery
Whenever possible, surgeons may use minimally invasive techniques.
Laparoscopic Surgery
- Small incisions and a camera-guided approach
- Less postoperative pain
- Shorter hospital stay
- Faster recovery
Open Surgery
- Required for severe obstructions or extensive scar tissue
- Allows direct access to the abdominal cavity
- Sometimes necessary in emergency situations
The choice of approach depends on the patient’s condition and the complexity of the obstruction.
Recovery After Surgery
Recovery varies depending on the severity of the obstruction and the type of surgery performed.
- Hospital stay typically ranges from several days to a week
- Gradual reintroduction of liquids and solid foods
- Walking soon after surgery to prevent complications
- Avoiding heavy lifting for several weeks
Patients who undergo minimally invasive procedures often recover more quickly.
Potential Complications
Possible risks associated with small bowel obstruction and surgery include:
- Infection
- Bleeding
- Recurrence of obstruction
- Damage to surrounding organs
- Postoperative adhesions
Close monitoring and follow-up care help reduce these risks.
Conclusion: Rapid Treatment Can Save Lives
Small bowel obstruction is a serious condition that requires prompt medical evaluation. While some cases resolve with conservative treatment, others require urgent surgical intervention to prevent severe complications. Advances in surgical techniques—including minimally invasive procedures—have improved outcomes and recovery times for many patients.
If you experience symptoms of bowel obstruction, seeking immediate medical care can make a critical difference in protecting your health and preventing life-threatening complications.
LENOX HILL MINIMALLY INVASIVE SURGERY LLP
155 East 76th Street
New York, NY 10021
Tel: 646-846-1136
Email: lenoxhillsurgeons@gmail.com